Rabies
17.1.1 Rabies What should an AHA do when an animal acts strange or crazy? What should they do after a wild dog has run through a village biting livestock and people? These are common situations for AHAs in areas where rabies is a problem.
Rabies is caused by a virus that affects the nervous system of all livestock, horses and people. (It does not affect poultry.) It is a frightening public health disease because after an animal or person gets sick from it, there is no treatment, and the disease is nearly 100% fatal.
Rabies is spread through the saliva of rabid animals, often by biting. Certain animals are known to spread rabies, such as dogs, skunks, bats and raccoons.
Caution: Many AHAs have been exposed to rabies when examining an animal’s throat because the animal appeared to have something caught in its throat!
65 The rabies virus moves from the bite wound to the brain, using the nerves as a pathway. This process usually takes 3 - 8 weeks, but in some cases, can take more than six months. Then the animal may begin to act strangely, appear weak, especially in its hind legs, and (due to paralysis in the throat muscles), drool, stop eating, and have a very odd-sounding voice. An animal with rabies may seem to have something caught in its throat.
When is the animal contagious?
The animal is contagious at the same time it has symptoms.
How do I determine whether someone was exposed? Anyone who was in contact with the animal’s saliva or nervous tissue (e.g. the animal’s brain tissue) should be considered “exposed”, especially if the saliva or nervous tissue was in contact with a wound or mucous membrane (i.e. tissue around the eye, in the nose, or mouth) of the person.
What can be done following exposure to rabies?
If exposed to rabies, wash the exposed area with soap and water (soap kills the rabies virus), and if possible, rinse with disinfectant. Then seek post-exposure rabies vaccination immediately. Do not wait for symptoms to appear. If a person or animal receives post-exposure rabies vaccinations before symptoms begin, the virus can be stopped before it reaches the brain, and the animal’s or person’s life can be saved. Once rabies symptoms appear, the person or animal will die.
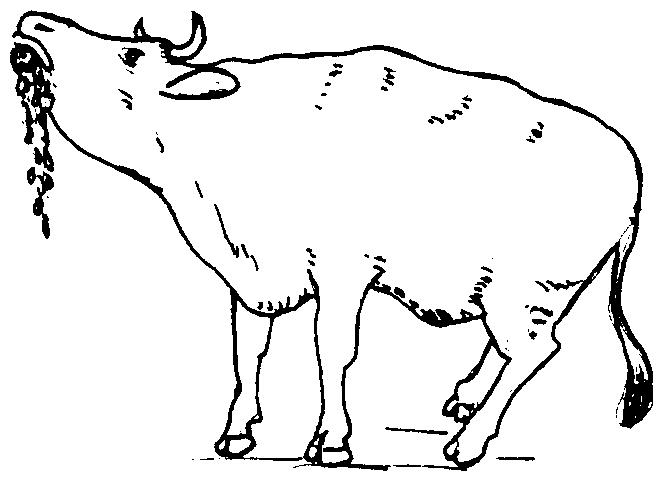
Symptoms: Symptoms vary. However, all animals show some change in behavior and most stop eating. Cattle often appear to have weak back legs. In general, an animal will show either “furious rabies” or “dumb rabies.” “Furious rabies” means that the animal acts aggressively. “Dumb rabies” means that the animal acts dull, listless, and weak. Sometimes their lower jaw may even hang open. All animals eventually become paralyzed and die. Most animals die within 4 or 5 days after the first symptoms appear. If the animal is still alive 14 days after the first symptoms appear, then the animal probably does not have rabies.
Diagnosis: A tentative diagnosis can be made based on symptoms and history. If there is a history of being bitten, and if rabies is common in the area, then assume that the animal has rabies. The diagnosis can be confirmed by carefully removing the animal’s brain (i.e. using gloves to avoid exposure to the brain tissue) and having a laboratory do one of the following three tests:
1. Fluorescent antibody: an accurate and rapid test, but one that requires fresh brain tissue that has been stored in ice.
1. Mousebrain inoculation: an accurate test that requires fresh brain tissue, but is less rapid than the fluorescent antibody test.
1. Negri body test: less accurate test (i.e. can miss some rabies cases), but the advantage is it does not require fresh brain tissue. That is, the brain can be placed in a solution of 50% glycerine or 10% formalin and transported long distances. However, since the test is less accurate, persons bitten by an animal should receive anti-rabies vaccination even if the test is negative.
In many remote areas, laboratory tests are impossible, and the following measures should be taken.
Wash all bite wounds thoroughly with water, soap and, if available, disinfectant!
66 Measures to take regarding a suspect rabies case (with no access to a laboratory for confirmation):
1. The bite wounds on the victim (livestock or human) should be thoroughly and immediately washed with water, soap and, if available, disinfectant. Use gloves when washing these wounds to avoid further exposure to the rabies virus.
1. All people bitten should begin post-exposure rabies vaccination as soon as possible. Note: If the bites are near the head, then it is even more urgent to receive post-exposure injections since the virus will travel more rapidly to the brain.
1. If the animal is acting deranged and aggressive, it should be killed as soon as possible to prevent further suffering and spread of rabies. At the same time, ensure that everyone exposed to the virus completes the series of post-exposure vaccination. Otherwise, catch the animal and chain it inside a secure pen to observe for 14 days. Continue to give the animal food and water. If it is still alive after 14 days, then rabies can be ruled out as the diagnosis and those persons receiving the post-exposure vaccination can stop doing so. If the animal becomes paralyzed and dies during the 14-day observation period, assume a diagnosis of rabies. Ensure that everyone exposed to the virus completes the post-exposure vaccination series. .
Vaccinations for Rabies There are many different kinds of vaccines used throughout the world. However, they are divided into two groups:
1. Pre-exposure vaccines are injections that are given at regular intervals (e.g. annually) before possible exposure to rabies. Consult a local veterinary officer for further information about what rabies vaccines are available in your area for livestock.
For wildlife, there are effective pre-exposure vaccines that can be given by leaving it in some food for the wildlife to eat.
2. Post-exposure vaccines are a series of injections that are given after possible exposure to a rabid animal. This series is usually effective in preventing rabies if it is given before symptoms begin in the person/animal exposed.
Control / Prevention: All dogs in the area should be vaccinated regularly with pre-exposure rabies vaccine. AHAs and their community can organize a vaccination clinic for all dogs. They can request help from the government vets.